-
+1 700 888 1234
-
Effingerstrasse 40 3008 Bern Switzerland
Therapy of lung cancer depends on its histological type and stage, but also on the presence or absence of biomarkers and the physical state. Treatments include surgical resection and chemotherapy. In general, patients with early-stage lung cancer are treated by surgery, and patients with advanced or metastatic disease by chemotherapy. Radiotherapy is used in some cases.
If the patient is a smoker, he/she should stop smoking. This is very important, because smoking can limit how well the treatment works. But the stress of having a cancer may make it more difficult to give up smoking. Doctors advise how, and they help patients to stop smoking.
Once doctors have verified that a patient has a lung cancer, and once they know the stage, they will propose a plan of treatment. Primary treatment is the main treatment used to eliminate cancer, and it can be surgery, chemoradiation, radiation therapy or a combination of these.
Treatments for lung cancer can produce side effects.
Surgery
When possible, surgery is used as the primary treatment in NSCLC. Surgery is not used in SCLC (in this type of lung cancer other treatments are used).
The surgeon will remove the lung tumour and lymph nodes. The tumour will be removed with ‘surgical margin’, which means that the tumour is removed together with some normal-looking tissue round its edge. The pathologist, in the microscopical analysis, will check whether there are cancer cells in the surgical margin, and whether there are cancer cells in the lymph nodes.
Chemoradiotherapy
In some stages of NSCLC, when cancer grew or spread outside the lung, cancer chemoradiation is used instead of surgery. Chemoradiotherapy means having chemotherapy and radiotherapy treatment together. Chemotherapy uses drugs to destroy cancer cells. These drugs circulate throughout the body in the bloodstream. And radiotherapy uses radiation over the lung to destroy cancer cells8. This treatment may greatly reduce the extent of cancer. After this treatment, there is a standard treatment with durvalumab, which may control cancer for a longer period of time.
Chemotherapy
The most common chemotherapy drug is cisplatin, which is often combined with other chemotherapy drugs. Usually chemotherapy is administered before radiotherapy starts, as a drip into the patient’s arm every 3 to 4 weeks. It might continue during the radiotherapy treatment, or when radiotherapy ends. Chemoradiotherapy can cause side effects, such as tiredness, sickness, a sore throat, and a cough and breathlessness.
The treatment of the small-cell lung cancer (SCLC) is by chemotherapy and radiotherapy (no surgery), as long as they can cover the entire area affected (tumour and lymph node). In other cases, the treatment is chemotherapy. The most commonly used drugs are cisplatin and etoposide. Radiotherapy is administered at the same time. Due to the high frequency of brain metastasis, a prophylactic cranial irradiation is recommended.
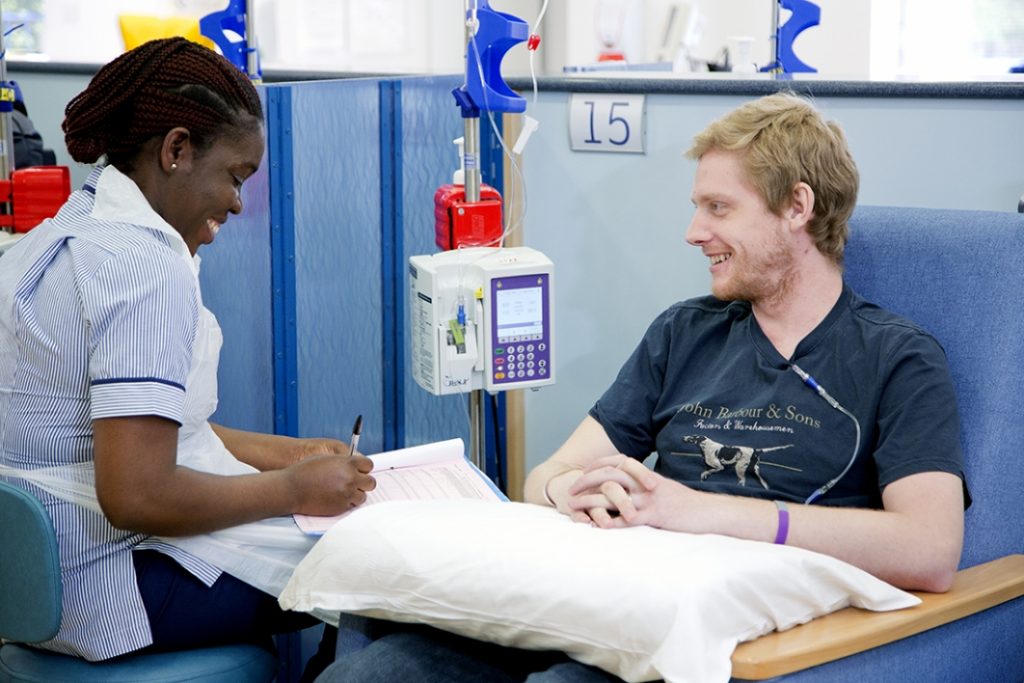
Figure. A patient receiving chemotherapy. The machine next to the patient’s arm is an infusion pump to give chemotherapy. These pumps allow patients to have chemotherapy in a controlled way. The infusion pump is capable of delivering fluids in large or small amounts, for a programmed period. Radiotherapy
Radiotherapy uses radiation over the tumour area of the lung to destroy cancer cells. In some stages, doctors can recommend chemotherapy after radiation, because chemotherapy can destroy cancer cells which the radiation did not destroy, as cancer cells spread to places outside the radiation field.
Instead of surgery, radiation therapy may be an option in some stages of lung cancer, when the cancer is only in lung tissue. If the cancer has grown or spread beyond lung tissue, it may be treated with chemoradiation instead.
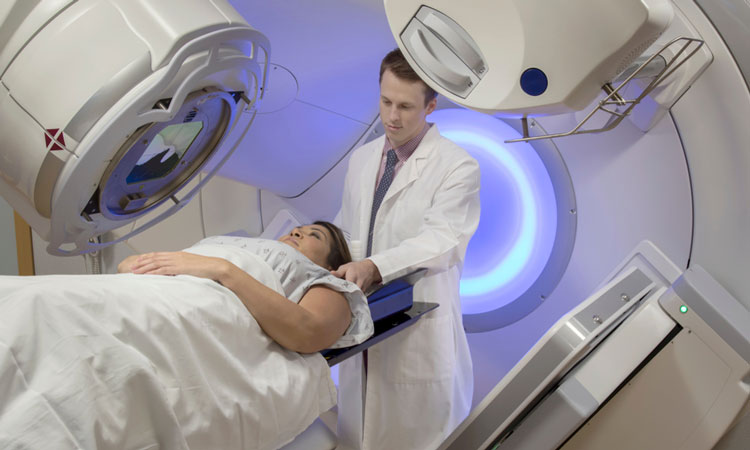
Figure. Machine for radiotherapy. Immunotherapy
Normally, immune systems recognise and fight cell cancers. But if the cancer appears, it is because the immune system has not worked properly to eliminate abnormal cells (cancer cells). Some immunomodulator drugs can help the immune system to recognise and fight cancer cells.
Some lung cancers produce particular proteins, such as PD-1 or PD-L1, which stop immune cells from recognising and destroying the cancer cells. There are immunomodulator drugs called checkpoint inhibitors which block these proteins. Once PD-1 or PD-L1 proteins are blocked, the patient’s immune cells can attack lung cancer cells. But checkpoint inhibitors do not work for all lung cancers, they only work for cancers with particular proteins.
Checkpoint inhibitors that have been approved by the EMA for some types of advanced lung cancer are atezolizumab, durvalumab, and pembrolizumab. (Another checkpoint inhibitor for lung cancer called nivolumab has been withdrawn at the request of the marketing authorisation holder). Several other checkpoint inhibitors are currently being tested in clinical trials for lung cancer.
Website Under Construction
We are currently rebuilding our website, and look forward to its launch later in 2026.
Until then, this website is not being updated. Feel free to continue browsing, or visit our news site for the latest updates.
